Unknown Chemical Exposure in Hospitals: Preparedness for Self-Presenting Patients
Unknown chemical exposure presents one of the most complex challenges in hospital emergency preparedness. Unlike coordinated hazardous materials incidents, hospitals often encounter patients who self-present to the emergency department after exposure, frequently without prior notification, confirmed substance identification, or activated emergency response systems.
These situations introduce immediate uncertainty. Hospital staff must make rapid decisions regarding triage, personal protective equipment (PPE), and decontamination procedures, all while managing the risk of secondary contamination within the facility. The combination of unknown chemical agents, unclear exposure levels, and the movement of contaminated individuals through clinical spaces creates a scenario where early actions determine whether the incident remains contained or escalates.
This blog explores how hospitals can strengthen preparedness for unknown chemical exposures, with a focus on self-presenting patients and the importance of early response.
What Happens When Patients Self-Present After Chemical Exposure?
In many chemical exposure incidents, patients do not arrive through coordinated emergency response systems. Instead, they walk into emergency departments on their own, often without realizing they may be carrying hazardous materials on their clothing, skin, or personal items.
This creates a scenario where the chemical agent is unknown, exposure levels are unclear, and hospital decontamination procedures are not yet fully activated. As a result, contaminated individuals may move through intake areas, waiting rooms, and triage zones before appropriate controls are in place. The emergency department becomes the first point of contact, and the first potential site of contamination, making early recognition and rapid containment essential to protecting staff, patients, and hospital operations.
Why Are Unknown Chemical Exposures So Challenging for Hospitals?
Unknown chemical exposures introduce a level of complexity that goes beyond standard hazardous materials incidents. Without knowing the substance involved, hospital staff must make rapid decisions without confirmed information about toxicity, volatility, or exposure risk.
This uncertainty affects multiple aspects of response. Selecting appropriate PPE becomes more difficult when the hazard is unclear, and triage decisions must balance immediate patient care with the need to prevent contamination from spreading further into the facility. At the same time, normal hospital workflows can be disrupted as staff work to isolate the patient, protect nearby personnel, and secure critical care areas.
Public health guidance and hospital preparedness frameworks emphasize that hospitals must be able to respond effectively even when key details are not immediately available. This reinforces the need for flexible, scalable response strategies that can adapt in real time.
What Does Emergency Preparedness Need to Address?
Effective emergency preparedness for unknown chemical exposure must account for how hospitals respond during the earliest moments of an incident, long before full decontamination systems or hazardous materials teams are activated.
Preparedness efforts should focus on how patients are received, assessed, and managed from the moment they enter the facility. This includes establishing clear intake and triage processes that help staff quickly identify potential contamination and isolate the patient before they move deeper into the hospital.
Staff must also be trained to recognize signs of chemical exposure, even when the specific agent is unknown, and to adjust workflows quickly to protect both people and infrastructure. Without these measures, a single exposure event can escalate into a broader incident affecting the entire facility.

Where Does Risk Occur During the First Minutes of Exposure?
The highest risk occurs in the first minutes after a patient arrives. Before full decontamination procedures are in place, contaminated individuals may pass through:
- Emergency department intake areas
- Triage and assessment zones
- Corridors and shared spaces
During this time, contamination can be transferred to surfaces, equipment, and personnel. Early actions taken during this window directly influence the extent of secondary exposure and overall incident impact. Hospitals must be prepared to act quickly to prevent hazardous materials from spreading beyond the initial point of contact.
Timing plays a defining role in how effectively hospitals manage unknown chemical exposure. Delays allow contamination to spread, increase health risks, and complicate both triage and treatment efforts.
Early intervention helps stabilize the situation, reduce uncertainty, and create a safer environment for both patients and healthcare professionals, even before the specific substance has been identified. Hospitals must have the capability to act immediately using tools and procedures that do not depend on chemical identification or complex setup.
How Does FAST-ACT® Support Unknown Chemical Exposure Response?
FAST-ACT® is designed to support hospital response during the earliest phase of a chemical exposure event, when timing, uncertainty, and risk are at their highest. Because FAST-ACT® does not require prior identification of the chemical agent, it provides immediate support for managing both vapor and surface contamination across a broad range of hazardous materials. This makes it particularly valuable in situations involving unknown substances.
FAST-ACT® can be used in key hospital areas such as emergency department intake, triage zones, and receiving corridors, where exposure risk is highest during the initial stages of an incident. Its dry formulation allows for use on sensitive equipment, helping reduce contamination without introducing additional operational challenges.
Common applications include:
- Rapid deployment using pressurized cylinders for broader contamination scenarios
- Targeted decontamination with mitts and wipes for localized contamination on skin or surfaces
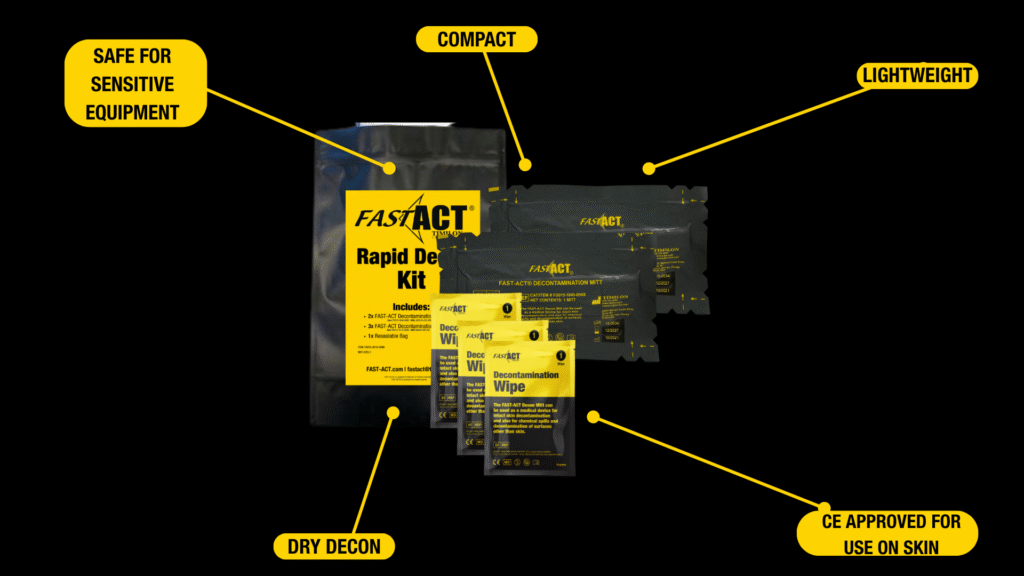
FAST-ACT® Decontamination Mitts and FAST-ACT® Decontamination Wipes are designed for safe use on skin and surfaces during early response, supporting flexible deployment in dynamic hospital environments. FAST-ACT® also offers comprehensive solutions such as the Rapid Decon Kit (RDK), which integrates pressurized application, mitts, and wipes into a compact, portable system, enabling hospital personnel and first responders to perform immediate dry decontamination and manage chemical spills without additional setup or equipment. FAST-ACT® is not a replacement for traditional decontamination procedures, but a complementary solution that helps bridge the gap between initial exposure and full system activation.
*Both products are CE classified as Class I medical devices for use on skin and surfaces in the EU.

How Can Hospitals Strengthen Preparedness for Unknown Chemical Incidents?
Strengthening preparedness for unknown chemical exposure requires a layered approach that combines structured protocols with practical early-response capabilities. Hospitals must ensure that staff are trained to recognize potential chemical exposure and respond effectively during the first minutes of an incident.
Preparedness should include clear role definitions for first receivers, designated decontamination areas near the emergency department, and ready access to appropriate PPE and early-response tools such as FAST-ACT®. Preparedness efforts must also consider how to maintain continuity of care while minimizing exposure risks, particularly during mass casualty incidents where multiple contaminated individuals may arrive simultaneously.
Unknown chemical exposure presents a unique challenge for hospital emergency preparedness, requiring rapid decision-making in situations where information is limited and risks are high. While hospital decontamination procedures and response protocols provide essential structure, their effectiveness depends on how quickly they can be implemented. The greatest vulnerability occurs in the early moments, before systems are fully activated, and contamination is controlled. By incorporating early-response solutions like FAST-ACT® alongside established protocols, hospitals can strengthen their preparedness strategies, reduce the impact of hazardous materials incidents, and better protect staff, patients, and critical operations.
About Timilon Corporation:
Timilon Corporation is the manufacturer of FAST-ACT®, a proprietary formulation of non-toxic high-performance specialty materials effective at neutralizing a wide range of toxic chemicals with the added capability to destroy chemical warfare agents. The FAST-ACT technology is utilized by leading defense agencies, chemical industrial companies, first responders and HAZMAT teams to quickly and safely eliminate chemical hazards. For more information, reach out to Leticia Menzzano, Marketing Manager, lmenzzano@timilon.com.
FAQs
How does FAST-ACT® support response to unknown chemical exposure?
FAST-ACT® supports early-stage response by enabling immediate dry decontamination without requiring chemical identification, water, or complex setup. It helps reduce vapor and surface contamination during the most critical phase of an incident.
Can FAST-ACT® be used in hospital intake and triage areas?
Yes. FAST-ACT® is designed for use in key hospital areas such as emergency department intake, triage zones, and receiving corridors, where exposure risk is highest during the initial stages of a chemical incident.
What FAST-ACT® products are used in hospital chemical response?
FAST-ACT® solutions include the FAST-ACT® 400g pressurized cylinder for rapid deployment, FAST-ACT® decontamination Mitts and FAST-ACT® Decontamination Wipes for targeted application, and comprehensive kits such as the FAST-ACT® Rapid Decon Kit (RDK), which integrates these tools into a portable system for immediate response.
How does FAST-ACT® differ from traditional decontamination methods?
FAST-ACT® is a dry decontamination solution that does not require water or extensive setup. This allows hospital personnel to act immediately, helping reduce contamination spread before full water-based decontamination systems are operational.



